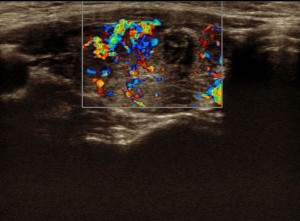
Insurance Information
Your hub for all the insurance forms and information.
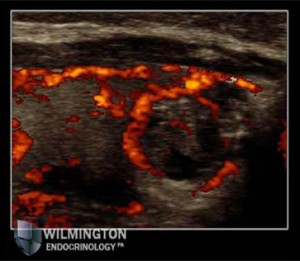
Insurance & Hospital Affiliations
We accept most major insurance companies including:
- Aetna
- Blue Cross Blue Shield
- Blue Cross Blue Shield – State Employees
- Cigna Healthcare
- MedCost Preferred
- Medicaid
- Medicare
- Tricare
- United Healthcare
Disclaimer: This list is updated frequently, but there may have been recent changes. Please call if you are unsure about any insurance options.
Hospital Affiliations
- New Hanover Regional Medical Center
- Cape Fear Hospital
Health Savings Accounts
If your employer provides you with insurance that has a high deductible, they are required to also provide a Health Savings Account (HSA). This is an account that you place money into. This money is deducted from your check. The following will show you how placing money into an HSA is the best way to prepare for medical expenses and will leave you with real money in your pocket.
- Money placed into an HSA is deducted before taxes are applied to your salary. Instead of paying the taxes up front to Uncle Sam, you benefit from the savings immediately. The equation is: Salary – Minus Your Contribution = Taxed Salary
- The money is then placed into an account that is usually accessed by a credit card. You pull this card out when asked to pay co-payments, deductibles and all sorts of out-of-pocket medical expenses for things like:
- Glasses & contact lenses
- OTC drugs ordered by your physician
- Visits to out-of-network doctors
- Dental visits and expenses
Start by computing the amount of medical expenses you have in a year. (Your last tax return will probably have the figure.) Medical expenses are only deductible if they reach 7.5% of your AGI (Adjusted Gross Income).
Most people lose out on this deduction because they do not meet this requirement — so why not get the deduction by placing pre-tax money in an HSA? You still get the standard deduction when you file your taxes.
Next you can divide the figure by the number of pay periods you have in a year to reach the per paycheck amount to contribute to your HSA. The following examples show how to compute your contribution and the effects of contributing to your HSA.
- Example: $1,000 expenses / 26 pay periods = $38.46 contribution per paycheck o A person who earns $500 per paycheck, is single and has one exemption, would have the following:
- Federal Taxes paid before contribution on $500 = $29 Gross $471.00 x 26= $12,246 – $1,000 medical expenses = $11,246
- Federal Taxes after contribution on $461.54 = $24 Gross $437.54 x 26 = $11,376 and the $1,000 medical expense was covered by the HSA
- You will profit $130 in this example with the HSA.
- Example: $2,500 expenses/ 26 pay periods $100 contribution per paycheck o Earns $1,600 per paycheck, married, two exemptions
- Federal taxes paid before contribution on $1,600 = $121 Gross $1,479.00 x 26 = $38,454-$2,500 medical expenses = $35,954
- Federal taxes paid after contribution on $1,500 = $106 Gross $1,394 x 26 = $36,244 and the $2,500 medical expense was covered by the HSA
- You will profit $290 in this example with the HSA
As you can see, because you paid the medical expenses out of your HSA account you retained more money in your pocket. During the year when you have medical expenses, you pay them with your HSA.
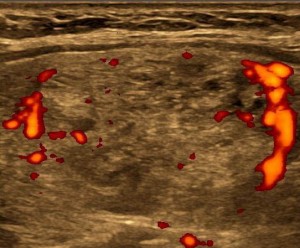
Coordination of Benefits
Sometimes more is just more, not better.
It used to be that having more than one insurance policy meant that you did not have to pay out of pocket for your medical expenses. Insurance companies have implemented measures that make this a thing of the past. Each insurance company applies different rules determining which insurance is primary and which is secondary. (One hopes the new healthcare legislation deals with this monster by creating a global rule.)
* First scenario… Husband and wife coverage. Both parties work. Most of the time your insurance from your job is your primary insurance and your spouse’s policy is secondary. So with two overlapping insurance coverages, this means that there will be no out of pocket expenses, right? Wrong. The primary insurance will be filed first and if there is a co-payment, deductible, or co-insurance, that amount is the responsibility of the patient. This claim is then filed with the secondary insurance which then determines what is the allowed amount for the claim. Then any amount paid by the primary insurance is subtracted from the total allowed amount. Next, if there is any balance, then co-payments, deductibles or co-insurances are applied. You may be paying for two insurance policies, and still not receive any benefit from them. Always know your policies. If you are deciding whether or not to get a secondary insurance policy, make sure it will cover ALL OF THE BALANCE REMAINING AFTER THE PRIMARY INSURANCE PAYS. Otherwise it may not be worth the extra premiums.
* Second scenario… Husband and wife coverage. One party retires. When an individual retires and has had a working history, at 65 he is covered by Medicare. At this point, Medicare becomes primary for the retired husband, and if he has additional insurance from his previous job (that he retired from), this insurance becomes secondary. If his wife is still working, her job insurance is primary and Medicare through him is secondary.
So, are we thoroughly confused yet? Here’s more.
Once one of the insurances declares it is primary, GET IT IN WRITING. Insurance companies have been known to make a complete about-face 2 years down the road and demand refunds from the doctor’s office, who will then bill you! This is usually what has happened if you ever receive a bill that is more than a year old from a physician’s office.

Pre-Existing Conditions
Insurance… it is constantly changing.
Here are some of the changes and what they might mean to you:
Insurance changes affect everyone. Over the past year the changes have occurred at a dizzying pace. Many insurance companies are now offering cheaper policies; however, this often means less benefits for the patient. The fact that you have a policy does not automatically assure you of coverage the next time you visit your doctor. You must take the time to understand the benefits of the policy and how the benefits (or lack thereof) affect you.
Most of the issues discussed here apply to OFFICE VISITS with a physician or specialist. Hospital coverage is another issue entirely. Always consult your policy documents for verification of the benefits that apply to you.
Pre-Existing Conditions
Many policies tack on a pre-existing condition clause. This is a waiting period during which any illness or disease that occurred before the insurance policy was effective may not be covered. If this clause applies, you may be responsible for the entire cost of treatment.
In order for your insurance company to categorize you as having a pre-existing condition, you must fulfill the following requirements:
- You must be over 18 years old. The newly passed health care reform laws do not allow minors to be assessed with pre-existing condition clauses.
- You must have a lapse in coverage of 60 days or more. When you discontinue coverage with an insurance company, that company provides you with a Letter of Credible Coverage. This letter proves to your new insurance company that you were covered until the date stated in the letter. If you can provide your new insurance company with this letter, that may cause them to have the pre-existing condition clause removed from your policy. Do not assume that because your previous coverage was with the same company, they know you were covered. You must notify the insurance company in order to have the clause removed. It is in your best interest to take care of this as soon as you acquire new insurance. If you did not have a lapse in coverage, then pre-existing condition cannot be assessed.
- You must have a condition that pre-dated the coverage with the current insurance company. This condition must have been treated by a physician and recorded in your medical records. The insurance company will send for medical records from all previous health care providers in order to verify whether this condition existed before you were covered. If you were never treated for the current condition, it is not a pre-existing condition and should not be assessed by the new insurance company. This does not mean that they will pay your claim immediately. Your claim may be delayed by their investigation into the pre-existing condition issue. However, if no treatment of the condition exists, they should eventually pay the claim.
If any one of the above items does not apply, you have escaped the pre-existing condition clause.
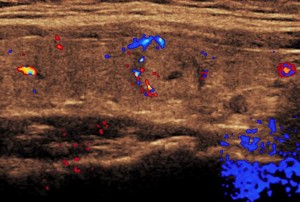
Deductibles & Co-Insurance
High Deductible Insurance
This type of insurance plan requires you to meet a substantial deductible before they will pay your claims. A deductible is the amount that a patient must spend before the insurance company will pay any benefits. Deductibles usually range from $250 to $10,000. If you have a deductible, you are required to pay for your visit until you have satisfied the deductible amount.
This office offers patients two methods of payment in these instances. You may:
- Pay the insurance-allowed amount in full at your visit; or
- Authorize charges to be applied to a credit/debit card once the claim has been adjudicated (settled) by your insurance company.
Co-Insurance
Co-Insurance is the split between the insurance company and the patient. It is the percentage that the patient will pay of the allowed charges. For a BCBS of NC member, if one has 20% co-insurance then they are responsible for 20% of the allowed amount of the charges. Wilmington Endocrinology PA office policy is that all deductibles, co-pays, and co-insurance amounts are due at the time of service. Estimates can be calculated for you before your appointment if you contact our billing department.